
Dubai as a dental hub: geography, market, and the formation of a transregional healthcare ecosystem
In the context of healthcare globalization, a key role is beginning to be played not by individual clinics or even
Main » Technologies » Robotic implantology: limits of accuracy and boundaries of autonomy in modern dentistry
The development of digital technologies in dentistry is gradually leading to the formation of a new clinical reality in which traditional surgical methods are complemented by intelligent navigation and automation systems. One of the most discussed areas in recent years is robotic implantology — a field at the intersection of surgery, engineering, and artificial intelligence. Despite its limited adoption, these technologies already demonstrate the potential to radically improve the accuracy and predictability of treatment, making them the focus of close attention from both researchers and practicing specialists.
The material under review, published in Dental Tribune International, allows for an assessment of the current state of robotic systems in implantology, their advantages, limitations, and prospects for further development in the context of digital transformation in dentistry.
Modern implantology has already gone through the stage of implementing static and dynamic computer navigation systems, which have significantly improved the accuracy of implant positioning. Robotic technologies represent the next stage of this evolution, combining the capabilities of digital planning with physical control of the surgical instrument. Unlike navigation systems that provide the surgeon with real‑time visual guidance, robotic platforms can directly stabilize tool movement and guide it according to a pre‑determined plan.
A key element of such a system is the integration of preoperative digital modeling with execution mechanisms, allowing deviations during osteotomy preparation and implant placement to be minimized. This provides higher accuracy compared to both manual techniques and traditional computer‑assisted methods.
One of the main arguments in favor of robotic implantology is the significant increase in the accuracy of surgical manipulations. Studies show that robotic systems can achieve minimal deviations in both the depth and angle of implant placement, which is critical for long‑term stability and the esthetic outcome of treatment.
High accuracy is particularly important in complex clinical situations, including limited bone volume or proximity to anatomically significant structures such as nerve canals and sinuses. In these conditions, even a minor deviation can lead to serious complications, making the use of robotic systems not just a technological advantage but a factor in improving clinical safety.
Despite the high level of automation, modern robotic systems do not imply full autonomy. Their operation is based on the principle of collaboration with the surgeon, who retains control over all stages of the intervention. As Professor Michael Bornstein notes, the robot should be viewed as an assistive tool, not a replacement for the surgeon, since it is the specialist who makes the key decisions and bears responsibility for the treatment outcome.
Thus, there is a transformation of the professional role: the surgeon becomes the operator of a complex technological system, monitoring the process and intervening when necessary. This shift requires new competencies, including understanding digital protocols, skills in working with navigation systems, and the ability to integrate technological data into clinical reasoning.
Despite impressive results, robotic implantology is at an early stage of development, which entails a number of significant limitations. One of the key factors is the insufficient number of clinical studies, since a significant portion of the available data comes from experimental settings or limited patient samples.
Furthermore, current systems are capable of automating only certain stages of the operation, primarily osteotomy preparation and implant placement, while more complex manipulations — including flap elevation, bone grafting, and suturing — still require manual execution. This limits the degree of technological autonomy and underscores the need to maintain a high level of surgical training for specialists. Additional barriers include the high cost of equipment and the complexity of integration into existing clinical processes, which hinders the widespread adoption of robotic systems.
The future of robotic implantology is largely related to the further integration of artificial intelligence and the improvement of control systems. It is expected that the development of data analysis algorithms will increase planning accuracy and system adaptability in real time, while improvements in mechanical components will expand the range of procedures performed.
In the future, it may be possible to extend the functionality of robotic systems beyond implantation to include more complex surgical interventions and work in limited‑access conditions, such as reduced mouth opening. However, even under this scenario, according to experts, technology development will occur within a collaborative rather than a substitutive model, where the robot serves as a high‑precision tool and the surgeon remains the key subject of the clinical process.
Robotic implantology represents one of the most promising areas of modern dentistry, demonstrating significant potential for improving the accuracy and safety of surgical interventions. Its development reflects the broader trend of medical digitalization, in which technology is becoming an integral part of clinical practice. The relevance of this topic is driven by the desire to minimize errors, increase the predictability of outcomes, and optimize treatment processes. Despite existing limitations, it is already clear today that robotic systems can significantly change the approach to implantation, shaping a new model of human‑technology interaction.
Thus, robotic surgery in dentistry should be viewed not as a replacement for the dentist, but as a tool that expands his or her capabilities and opens new horizons of clinical precision, ultimately contributing to improved quality of medical care and better patient outcomes.

In the context of healthcare globalization, a key role is beginning to be played not by individual clinics or even
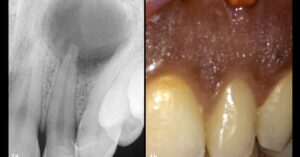
One endodontic system, multiple motions: case-based approaches to routine challenges Introduction / background Root canal anatomy and its variations remain


OTEXE.COM uses cookies to personalize the services and improve the usability of the site. If you do not want to use cookies, please disable them in your browser settings.
We use cookies to improve website performance, analyze traffic, and personalize content. You can accept all cookies or customize their use. Learn more in our Cookie Policy.
